
BLOG
Our health stories

Can the Theory of Constraints aid in managing our healthcare bottlenecks?
In a healthcare system, the application of the Theory of Constraints could be highly beneficial for streamlining processes, improving patient outcomes, and maximising resource utilisation.

What role does the digital and healthtech industry sector play as part of the wider health reform
One current challenge in healthcare delivery is the unequal distribution of healthcare resources, leading to disparities in access and quality of care. Unifying the system can help address this challenge by providing a single system that ensures equal access to healthcare services for all individuals, regardless of their socioeconomic status or geographic location.

How can New Zealand use digital health strategies to align the healthcare system with modern needs?
Over the past decade, it has come to light that healthcare IT infrastructure networks, and security are outdated and unable to adequately support the introduction of new systems or manage increased cybersecurity issues. This outdated infrastructure also presents challenges to users accessing and using patient or clinical information across both internal hospital locations and wider health service settings.
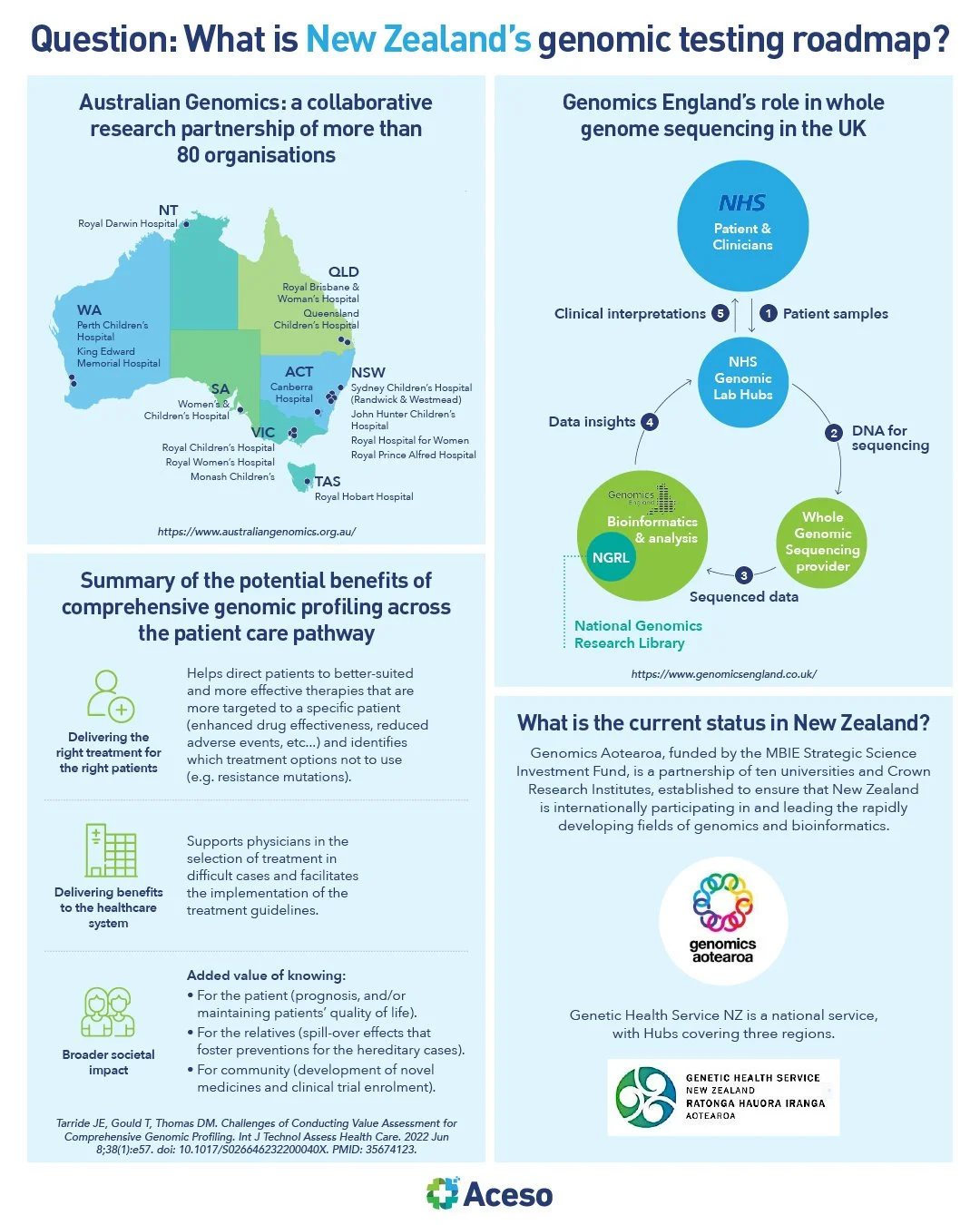
What is New Zealand’s genomic testing roadmap?
Over the next few years, genetic testing will become more available and more affordable. Combining this with ongoing research around precision health, and we will begin to see clinical applications emerge. In parallel, we will require national policy and government regulations to form supporting guardrails that enable progress and protect New Zealanders.

What is the value of infrastructure investment in securing the future of New Zealand’s healthcare sector?
Investments in infrastructure for health can be costly and seem untenable in resource constrained settings. These investments compete with other equally important areas. Nonetheless, infrastructure investments can contribute substantially to alleviating burdens of morbidity and mortality while also providing a positive return on investment in the long term.

New Zealand’s aged care sector is under threat. How do we find sustainable, long-term solutions for the industry?
New Zealand is not alone in facing an ageing population dynamic and difficulties in meeting the workforce required for aged residential care. It is of sufficient policy concern that the OECD has a Long Term Care work programme to address related policy concerns. According to experts, the sector is doing everything it can to maintain viability, however we will need to revisit the funding model, revisit how to address the workforce shortages and commit funding over many years, to find sustainable long-term solutions for the industry.

How do we better support rural hospitals in the New Zealand healthcare system?
Rural hospitals are well placed to provide an integrative role in locality service provision, with many already long established in performing this role. It would be very remiss of the wider sector to undervalue the importance of the rural health system, its challenges and needs.

What can New Zealand learn from experiences in other countries around personal health records?
Most countries face an ageing population, increasing prevalence of chronic diseases and experience an ever tightening budget for providing health services. Involving patients in their own care by allowing them access to their patient data is a trend seen in many places. A number of commercial solutions that allow individual users to gather, store, use, and share health information are offered globally. It is, however, noticeable that only a few countries' governments have offered citizens access to their own health data on a national level.

How do we overcome challenges in providing high quality online information on common health conditions and healthy lifestyles for patients and whānau in New Zealand?
Partnerships of academic institutions and governmental agencies are needed to establish quality standards and develop a monitoring system for online health information producers to reduce healthcare waste and improve health outcomes.

How can the wider New Zealand ecosystem augment the strong clinical trials sector?
Future investment in clinical trials is likely to continue to produce large health benefits. Prioritisation of trials should be based on factors such as disease burden, gaps in health outcomes between different populations, and include those areas where there may be potential to have a greater impact and return on investment.

How do we effectively utilise co-response teams in healthcare across New Zealand?
Despite favourable evidence, the implementation of such teams has also been criticised. A systematic review of CRTs found a lack of evidence to evaluate their effectiveness; they found wide variation in the implementation of these teams, differences in hours of operation, staffing, and incident responses. Another criticism of CRTs includes a possible increase of the pressure on already stretched police and mental health services, making adequate resourcing crucial.

Why are we experiencing a rise in medication dispensing to young adults in New Zealand?
There are a range of ways in which young people can and need to be supported. There is good evidence for regular physical activity, good nutrition, and adequate sleep. Support from family, schools and the broader community is also important. A decision to use medications should be on the basis of shared decision-making.

Treating cancer is only part of the journey. How do we improve the rest of the journey for patients and families in New Zealand?
We have many world class aspects of cancer control in New Zealand, and the cancer workforce is full of highly committed and talented people, but if we are to improve our cancer survival rates compared to similar countries, focused action is needed

How do we achieve equitable access to medicine in New Zealand?
By failing to invest, New Zealand misses out on the savings to the health system and economic benefits that modern medicines offer. With this in mind, how do we make improvements to safeguard the future of our healthcare sector?

Data and insights that help governments prioritise health challenges and allocate resources, rely on robust country-wide health information systems. How is New Zealand tracking?
Transparent, accurate and accessible information enables patients and the public to know whether the services they are receiving are high quality, efficient and effective. Equally, clear and effective engagement with the public builds confidence that individuals’ data contributions are creating real benefits for themselves and wider society, thus underpinning further improvement and transformation.

Women and health are key to sustainable development. In July 2023, New Zealand will share its first ever Woman’s Health Strategy. What can we expect from it?
While Aotearoa is a relatively progressive country regarding women's health, there are still barriers that women face in accessing healthcare and achieving optimal health outcomes. The countries that perform best in terms of women’s care outcomes have high levels of gender equality, access to healthcare, and other social and economic factors that contribute to women's well-being.

How can New Zealand attract the finite healthcare workforce resource?
Health systems can only function with health workers; improving health service coverage and realising the right to the enjoyment of the highest attainable standard of health is dependent on their availability, accessibility, acceptability and quality.

How do we create a fit-for-purpose regulatory framework for digital health in New Zealand?
The rapid uptake of such digital tools points to an area ripe with opportunity to improve and complement existing health care services and reach historically underserved populations. But to fully realise the benefits of novel digital offerings, concomitant innovation in regulatory pathways is necessary.

How do we improve healthcare rehabilitation pathways in New Zealand?
Are we are stuck dependent on an under-funded and inefficient system that could be preventing people from reaching their full potential unless they have the means to do it themselves?

What is the changing role of allied health professionals in New Zealand’s evolving healthcare landscape?
It might be worthwhile to begin with answering the transdisciplinary riddle: What is it that you do and you need to do and only you can do, as opposed to what is it that you do, that needs to get done, but you do not necessarily need to do?
